
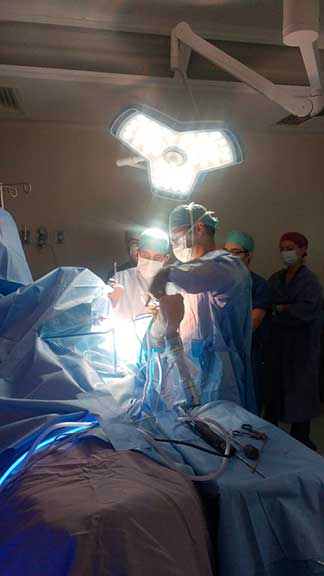
It allows to see the shoulder joint through three portals smaller than one centimeter in diameter which allows to corroborate the diagnoses and apply curative treatments since most of the structures of the shoulder are accessible by arthroscopy. It is a minimally invasive technique to access the two compartments of the joint, the glenohumeral and subacromial.
It is a treatment option in rotator cuff pathologies (supraspinatus, subscapular, infraspinatus and round major), tendonitis of the long portion of the biceps, subacromial compressions, glenohumeral instability and some types of fractures or dislocations.
A shoulder immobilizer should be used for three to six weeks, physical therapy is essential for post-surgical success which should be constant for a few weeks and reach the goal of recovering function without pain and with adequate strength.
Being a minimally invasive technique, postoperative pain is low, it allows us to transfer home early and prompt integration into physical therapy, which would help us reintegrate the patient to the normal use of the previously damaged shoulder in a few weeks after surgery.
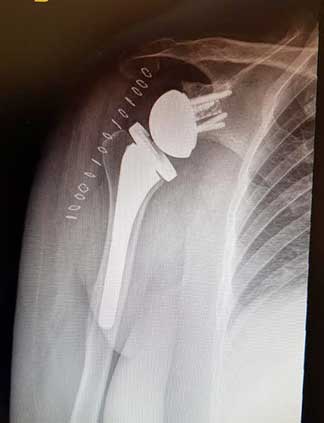
It is the artificial replacement of the joint by a metal and polyethylene implant indicated by osteoarthritis, wear or massive injury to the rotator cuff.
Its main indications are fractures of the proximal limb of the humerus, glenohumeral osteoarthritis and rheumatoid arthritis, although in recent years reverse shoulder prostheses are being shown as an effective option in the treatment of shoulder arthropathy associated with a massive and irreparable rupture of the rotator cuff.
It is an artificial joint that replaces the injured shoulder that cannot be cured with less invasive techniques.
The intention of a shoulder surgery is to improve the function of the joint, as well as to recover the functional arches of movement without pain and equated to the resistance and strength prior to the injury. The recovery of shoulder replacement surgery with a reverse shoulder prosthesis or an anatomical shoulder prosthesis is closely linked to the state of the previously injured joint and the attachment that the patient has with physical therapy and thus be able to offer a good, very good or excellent recovery.
Loss of continuity of bone tissue from the shoulder joint, acromioclavicular joint or shoulder girdle, which are made up of humerus, scapula and collarbone.
The treatment can be surgical or conservative (non-surgical) which will be determined by the characteristics of the patient, the fractured bone and the displacement of the fragments, which may consist of immobilizations or open, minimally invasive or arthroscopic surgeries.
It is necessary to take care of osteosynthesis of the shoulder for weeks after surgery, adhering to frequent physical therapy to avoid the pain of edema and post-surgical stiffness. Protocols for surgical shoulder rehabilitation are very well protocolized and standardized to improve outcome and range from 4-12 weeks.
As for shoulder fractures, that is, of the proximal humerus, scapula or glenohumeral joint, it is important to always consider the degree of the injury, that is, the complexity of the number of bone structures and whether it affects the joint, and if it is a fracture with multiple fragments. But the intention of a surgery is always to achieve the best functional result to improve the quality of life of the patient.
Fluoroscopic image of a female in her third decade of life, who had a wrist fracture while practicing mountaineering. an anatomical miniplate can be seen.
Ankle arthroscopy
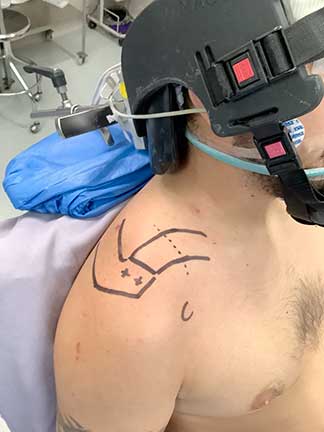
Minimally invasive approach. in a female patient operated on for reduction of a wrist fracture with an anatomical plate.
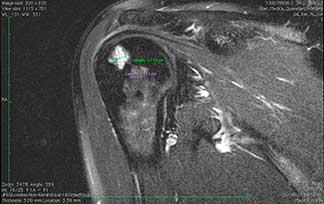
Ankle osteoarthritis grade IV, arthroscopic vision